Radiosurgery
What is the HALLMARK of the Center's radiosurgery department?PetCure Oncology at VRIC is on the leading edge of cancer care for your patients thanks in part to an advanced radiosurgery machine designed to deliver Stereotactic Radiosurgery (SRS). Only a handful of hospitals in North America have our capabilities! This is the latest in radiation oncology, paralleling only the most advanced human hospitals. Our staff is a dedicated group of highly skilled veterinarians, technicians, radiotherapists and other professionals who strive to deliver the best in veterinary medical care.
Dr. Neal Mauldin, a leader in the veterinary oncology field, constructs each treatment plan. We have radiotherapists from the human sector who deliver each fraction. We take pride in providing patients and clients with a high level of attention in a warm and caring environment. Many of our "graduates" return months (and years!) later just to say "Hi!" A supportive, caring community is one that heals.
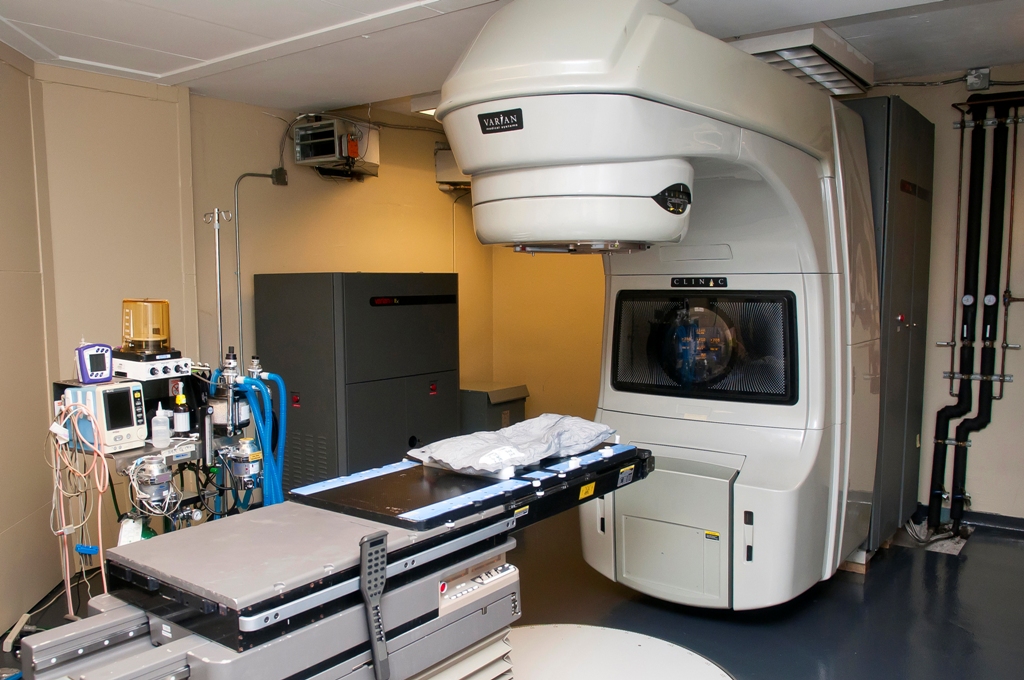 What is radiation?
What is radiation?
Radiation therapy is a form of treatment that causes localized DNA damage and ultimately, cell death.
What is SRS?SRS, or stereotactic radiosurgery, is a highly focused form of radiation therapy delivered with submillimeter accuracy. SRS delivers curative intent doses of radiation in 1-3 treatments (fractions) given on consecutive days, treating patients in one week or less. Fewer anesthetic events are necessary and typically much less acute toxicity is seen than with conventional RT. Surgery (mass removal) should NOT be performed prior to this modality of treatment.
Indications: Tumors that are responsive to SRS- Oral Melanomas
- Squamous cell carcinomas
- Fibrosarcomas
- Plasmacytomas
- Acanthomatous amelioblastomas
- Adenocarcinomas
- Nasal Tumors
- Meningiomas
- Pituitary Tumors
- Osteosarcomas
- Soft Tissue Sarcomas
- Fibrosarcomas
- Infiltrative Lipomas
- Mast Cell Tumors
- Spinal Tumors
- Anal Gland Adenocarcinomas
- Bladder Tumors
- Prostatic Tumors
Head and neck
Brain tumors
Thyroid Tumors
Extremity Tumors
Pelvic Canal Tumors
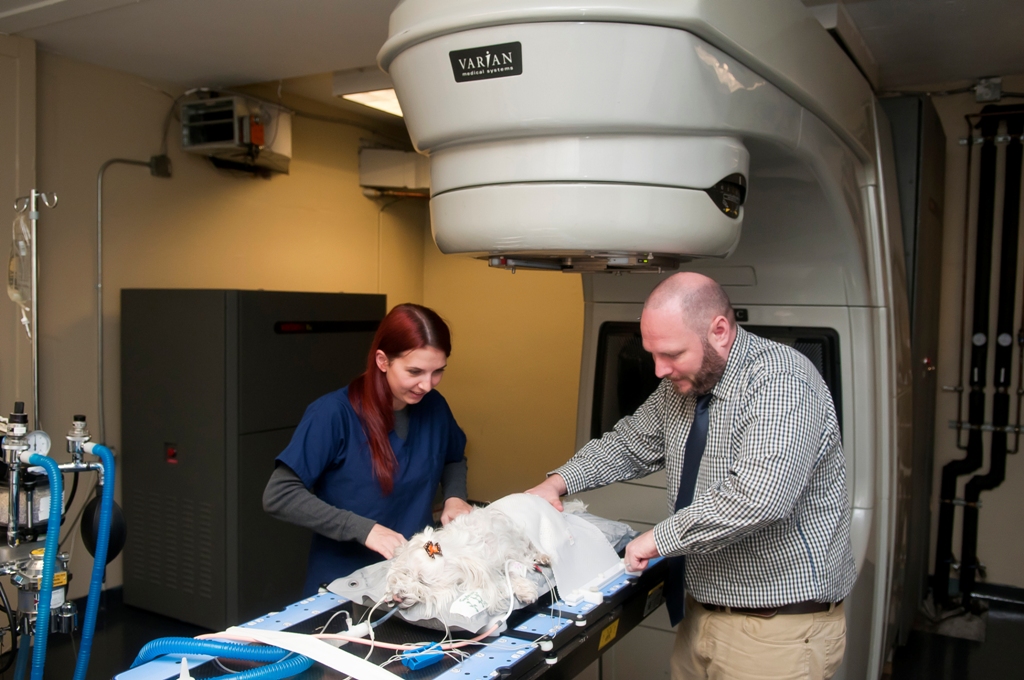 How does radiosurgery work?
How does radiosurgery work?
Radiosurgery primarily kills neoplastic cells through a reproductive death. Radiation causes ionization of atoms that directly damages the target tissue's DNA. This can further result in free radical formation, causing further damage to the target tissue. While the cell has sustained such damage, it is not until that cell divides that it, in fact, dies (hence a reproductive death). This is of importance in treating various neoplasms. Some tumors have a very quick doubling time and growth fraction. These tumors would seemingly respond faster than those that are of slower growth. Although less common, apoptosis is a second avenue of cell kill. These cells would experience a very rapid response to radiation. This includes lymphocytic tissues (lymphoma) and also the lacrimal gland.
What is palliative radiation?Most cancers are treated in a definitive manner with radiosurgery. This would be with the intent to cure the patient, though sometimes only remissions can be obtained. Palliative radiation is therapy with the intent to improve quality of life, though not altering/increasing lifespan. A prime example of palliative radiotherapy is seen with appendicular osteosarcoma. Should a patient with osteosarcoma not undergo surgery, palliative radiotherapy can greatly decrease pain associated with such a tumor. Some treated dogs will no longer need pain medication, others a mere reduction in medication, for an improved quality of life.
What types of cancers can it help?It was initially thought that radiation primarily benefits those tumors with a short doubling time and high growth fraction. These cancer types include lymphoma, mast cell tumors, transmissible venereal tumors, plasmacytomas, melanoma and many carcinomas. However, at higher doses, soft tissue sarcomas (once thought to be radioresistant) are quite treatable. Radiosurgery is frequently the modality of choice for brain tumors.
How do I refer a case for radiosurgery?Any case is welcome for evaluation for external beam radiosurgery. A case must be seen by a board certified veterinary oncologist to receive radiotherapy. A full work-up (see below) is not necessary for the initial evaluation, but may be recommended after consultation. Should you or your staff have any questions regarding a radiation case, please do not hesitate to contact any of us by phone. We are happy to help!
What are the side effects?Radiosurgery affects only those tissues that are in the treatment field. It can have both acute and late sequelae. Not all pets will experience adverse reactions. Some may only experience mild side effects. Tissues do not "glow" and will not emit further radiation. It is safe for owners, the elderly and children to be around a pet that seconds ago received treatment.
Acute toxicity is seen in rapidly dividing tissues. Cutaneous burns can result in slightly to moderately reddened, sore skin. A dry or moist desquamation may occur. Conversely, hyperpigmentation may develop as permanent sequelae. Should the oral cavity be in the field, mucositis can occur. Acute ocular toxicity can include conjunctivitis, and/or keratoconjunctivitis sicca. KCS would be a permanent condition, as the lacrimal gland goes not regenerate. Every effort is made to attempt to decrease these side effects via the patient's set up, treatment schedule and/or with medications.
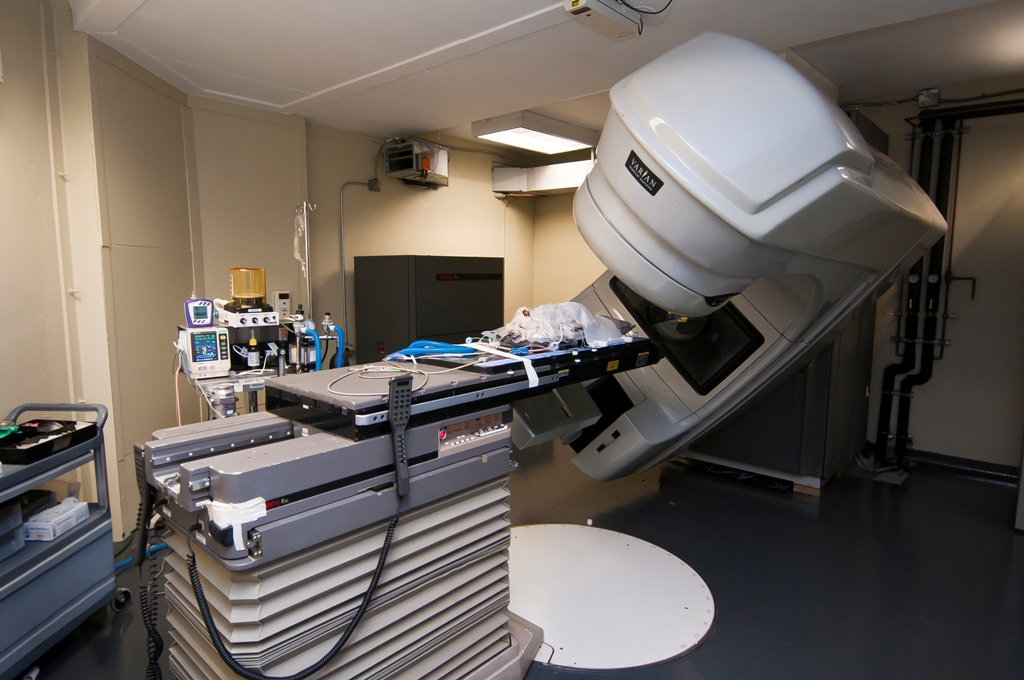
Late toxicity is much less common than acute. Late toxicity is seen in slowly dividing tissues. While infrequent, it can develop 6 – 12 months post- treatment. Fibrosis of muscles has been reported in the literature, but is not seen much clinically. Strictures of structures in the treatment field (i.e. esophagus, rectum, etc.) can develop. These may never be clinically relevant or could cause morbidity to the patient. Fur in the field may never grow back and fur that does will often grow back white. Late sequelae to the eyes include possible cataract formation, retinal degeneration, corneal damage and blindness. Should the CNS be treated, scar tissue may develop, causing a seizure focus. If the heart or lungs received a moderate dose of radiation, fibrosis (restrictive pericarditis, pleuritis) can also occur. Lastly, secondary cancers can develop in and from the treatment site. This is reported in 2 – 5 % of patients receiving radiation to the oral cavity. Precautions such as lead shields, treatment field manipulation and various medications are employed to minimize these potential late effects.
Why does a pet need a radiation simulation?Prior to receiving multiple fractions of radiation, a set up, or simulation is necessary. At this time, the patient is anesthetized or heavily sedated. The animal is placed on the machine at various positions to assess the best position for that patient to repeatedly receive treatments. Tumor target measurements are made and mathematical calculations are done to obtain the best dosing scheme for the pet. CT scan may be employed for more complex treatment fields and for more accurate planning purposes. The patient is typically marked with indelible ink for future guidelines to reproduce the set up throughout the pet's treatment. Polaroids or digital images are frequently taken and secured to the patient's treatment chart to help visualize and recreate the set up.
What tests are required before radiosurgery?As with any cancer, it is important to make sure that a patient does not have metastatic disease before initiating therapy. As radiation is only a local treatment, in many instances it would be inappropriate to treat an animal with systemic disease solely with radiation. However, radiosurgery may be used in concert with other modalities (i.e. chemotherapy, surgery) for systemic disease or with a palliative intent.
Prior to beginning radiation, a thorough history and complete physical exam should be performed. A CBC, chemistry profile, urinalysis and three view thoracic radiographs should be obtained to assess for other diseases, rule out metastasis and help insure that the patient is a good candidate for sedation or anesthesia. A thoracic CT should also be considered as we have seen cases where thoracic radiographs are normal and metastatic disease is found on a CT scan. A definitive diagnosis (via histology or cytology) should be obtained. Lymph node aspiration should be considered. Treating "presumptive" neoplasia could result in an adverse reaction for the patient (sepsis). Lastly, a CT scan is often very useful for staging and treatment planning purposes. CT allows complete visualization of the tumor bed and, through computers, a much more detailed treatment plan can be created.

